
Care for safety - Safety of persons with a serious mental illness and their environment
In the Netherlands there are 250,000 to 300,000 persons with a serious mental illness (SMI). About 20,000 of them need acute care because of their condition. The problems of vulnerable persons with an SMI are often chronic, multiple and episodic. Because of this fragmented system, in complex situations the focal point is not the person with an SMI but the organisation offering the care. The Board investigated, among others, seven cases where safety is at risk.
Access to adequate care
The Dutch Safety Board has observed that unsafe situations for persons with an SMI and their environment occur frequently. This is why the Board investigated which factors contribute to the development of such situations. The Board has concluded that the safety of both vulnerable persons with an SMI and their environment is insufficiently secured. Among other reasons, this is because the care and services provided to this group of people does not meet their care needs sufficiently. Vulnerable persons with an SMI also tend to have problems with their relationships, housing, finances, work and physical health. These problems are largely episodic in nature. This makes them dependent on their social environment as well as on mental health and social workers at different moments, in different life areas and to varying degrees. Because of their mental disorder these individuals are not able to effectively take the reins of their situation. When they cannot take care of themselves, for example during a crisis, someone else needs to protect them and take over these responsibilities from them.
To increase the safety of persons with an SMI and their environment, it is necessary for the care and support to fit with the complex and episodic care needs of individual patients. To this end, financial restrictions in laws and regulations should be removed. This can be done by widening access to existing financing resources, such as opening the Long-Term Care Act to vulnerable persons with an SMI, as well as by experimenting with new, domain-transcending financing resources. Mental health and social workers also need to take more advantage of their professional latitude to secure the safety of persons with an SMI and their environment. This requires that professional groups, institutions and care professionals from the various domains discuss how to detect, exchange and manage safety risks earlier, as well as recognise and openly discuss dilemmas that affect the safety of patients and their environment. Lastly, mental health and social workers should also be supported to a greater extent in their ability to take responsibility for offering personalised care to individuals with an SMI. To this end, it is necessary to make it easier for mental health and social workers to accumulate sufficient knowledge and skills, to assist them in dealing with dilemmas and to structure the preconditions for them to want to, be able to and dare to offer personalised services.
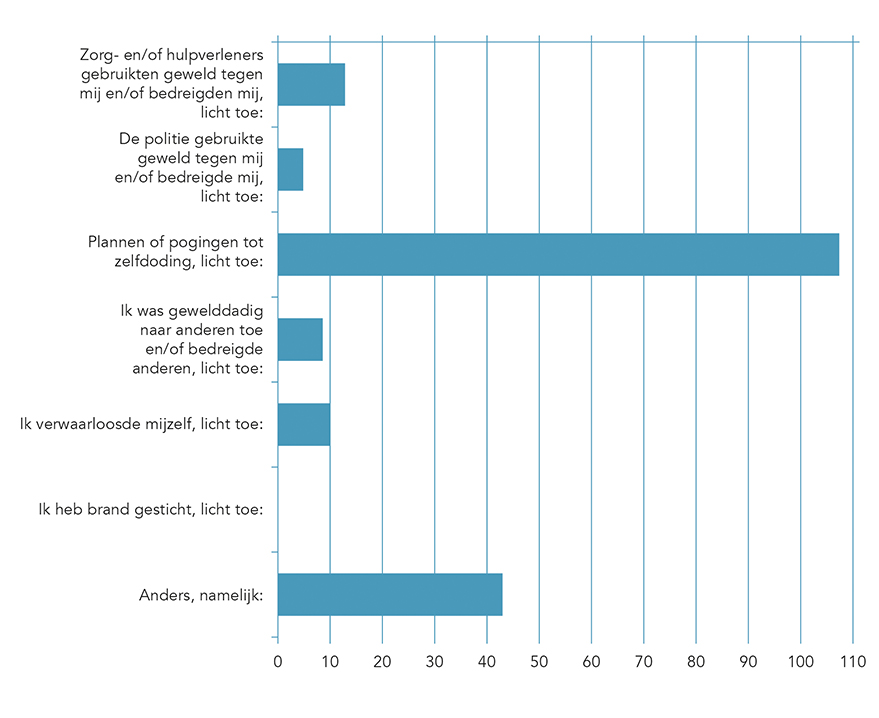
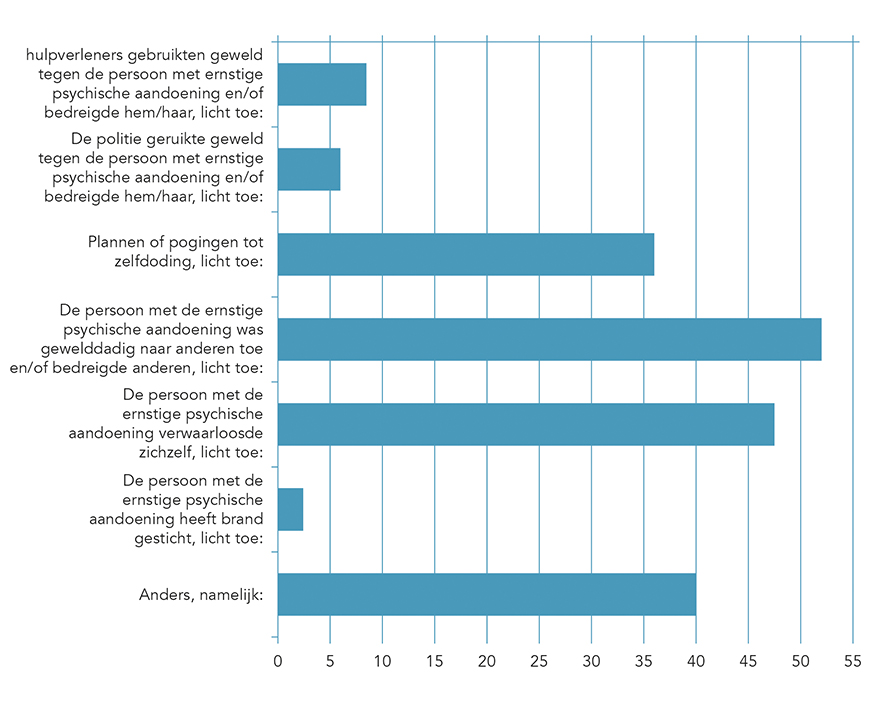
Related news
-
News:
Study into safety, care and support for persons with a serious psychiatric disorder
- General
- Healthcare
